Information & Documents
Patient Procedure Documents
We need to make sure that your procedure is appropriate for you.
If you are scheduled for a stellate ganglion block, you must complete a PCL-5 and a basic medical questionnaire. If you are scheduled for IV infusion therapy, you will only need to complete the basic medical questionnaire. If you are scheduled for TMS therapy, you will only need to complete the basic medical questionnaire.
After we have discussed your procedure, its potential benefits, and its potential risks, and you have had your questions answered, you will need to sign an informed consent.
What to expect and how to prepare for your SGB or IV Drug Infusion Therapy Procedure
Let us know during your consultation if you are taking anticoagulant medication (blood thinning medication that prevents you from forming blood clots), and we will discuss when to stop taking them before the procedure. Also, let us know if you have any allergies to medicines. Do not eat or drink after midnight on the day before the procedure unless instructed otherwise.
On the day of the SGB procedure
On the day of the procedure, you will need to arrange for a driver to take you home. If you are having an SGB, wear a top that you can remove easily or one that will completely clear the right shoulder and neck. Wear a loose-fitting short sleeve top. If you would prefer, a loose-fitting gown can be provided. Remove any necklaces or large earrings. After an SGB, your right eye will look droopy for about 4-8 hours after the procedure, so do not schedule any important photos of your face on that day.
During the SGB procedure
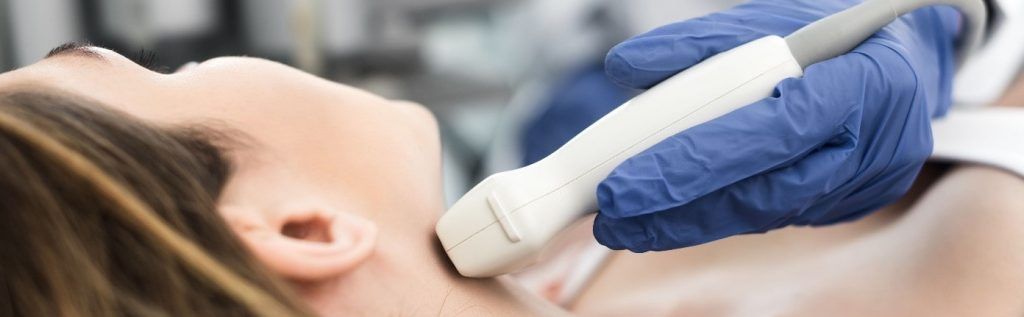
You will lie face up on our treatment table with your right shoulder and neck exposed. An intravenous catheter (IV) will be inserted, and a saline solution will be started. The skin on your right shoulder and neck will be cleansed with an antiseptic surgical skin preparation and sterile ultrasound gel applied to the neck. The right side of your neck will then be scanned with ultrasound, and the collection of nerves will be identified.
Once the nerves have been identified, medication for sedation will be administered as indicated (most patients will require some level of sedation), and a small amount of local anesthetic will be injected into the skin to make the procedure more comfortable. The needle will be guided to the stellate ganglion using real-time ultrasound guidance. Once the needle is at the target, a long-acting anesthetic will be slowly injected over 2-3 minutes.
During the injection, Dr. Garwin will ask if you are doing ok, if you have a metallic taste in your mouth, or if there is ringing in your ears. It will be safe to answer questions. Otherwise, you should refrain from talking or moving during the procedure. Once the needle is removed, you will lie flat for 5 minutes. Then you will sit up and have your SGB assessed.
When an SGB is performed, and the sympathetic nerves are blocked, we are looking for a temporary condition referred to as “Horner’s syndrome”- your right eyelid will be droopy, your right pupil will be smaller than the other pupil, and the white part of your right eye may get red. This condition is a normal part of the block and will wear off in 4 to 8 hours. After the procedure, a provider will observe you for 30-45 minutes before being allowed to go home.
After your SGB procedure
Plan on taking it easy for the rest of the day. You should not drive or operate heavy machinery on the day of the procedure. Following the procedure, you may eat whatever you feel you can tolerate, but you should begin with liquids.
Fill out another PCL-5 questionnaire and email it to the Albany Clinic at contact@thealbanyclinic.com one week after your injection so that we can track how you responded to the SGB. Many patients get sustained relief from their symptoms and do not need further treatment, but in some patients, symptoms may be retriggered and recur. If this happens and the block helped you previously, the SGB may be repeated. Do not let your symptoms fully return before seeking treatment.
If you notice a regression of your symptoms, seek help by calling the clinic or contacting your mental healthcare provider. SGB is not intended to be a standalone treatment for significant PTSD. It needs to be part of a treatment plan integrated with other modalities by your mental healthcare provider.
In the event of complications
Although complications with SGB are exceedingly rare, if there is pain that is getting worse in your neck or you experience shortness of breath, these could be signs of a more severe complication. If this should occur, you should contact 911 or go to your local emergency room and tell them that you had an injection in your neck performed that day. Most people feel the results of an SGB within an hour. Keep track of the symptoms that were bothering you and make note of any differences.
During the IV Drug Infusion Therapy Procedure
You will be seated in a reclining chair, an IV catheter inserted, and a saline infusion started. Monitors will be applied, and oxygen will be administered. The IV Drug Infusion Therapy will be initiated through the IV catheter and will require 45 to 60 minutes to complete. Most patients will drift off to sleep during the infusion and be awakened after the procedure.
After your IV Drug Infusion Therapy
Most patients get substantial relief almost immediately after receiving IV Drug Infusion Therapy. Monitor the symptoms that were bothering you and make note of any new or different symptoms. Contact us within a few days following your infusion so that we can track your response to treatment.
Some patients may get sustained relief from their symptoms and will not need further treatment, but patients often require more than one IV Drug Infusion Therapy, especially if their symptoms are retriggered or recur.
If you notice a regression of your symptoms and want another drug infusion, seek help by contacting the clinic or your mental healthcare provider. IV Drug infusion therapy is not intended to be a standalone treatment for Treatment-Resistant Depression. It needs to be a part of a treatment plan integrated with other treatment strategies by your mental healthcare provider.
In the event of complications
Complications with IV drug infusion therapy are extremely uncommon. However, you should still be alert. After an IV Drug Infusion Therapy, if you experience worsening psychological symptoms or suicidal ideation, contact 911 or go to your local emergency room.
During TMS procedure
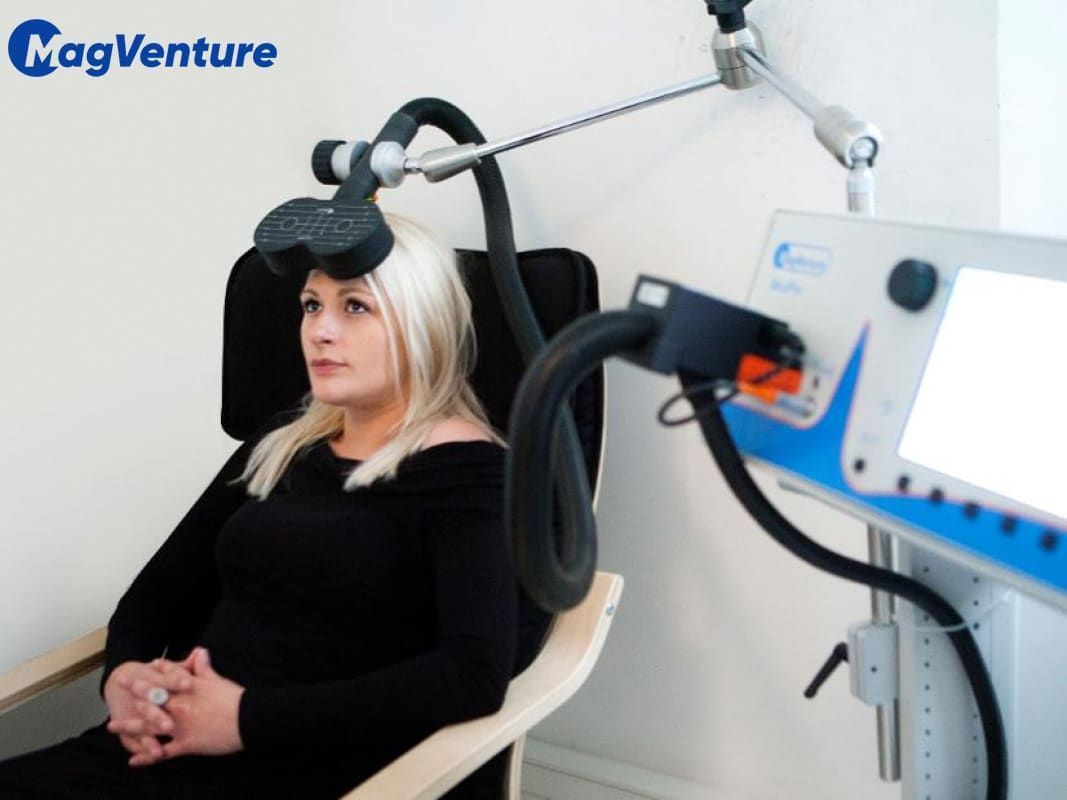
TMS is a relatively short, noninvasive, non-drug, brief treatment typically done in the convenience of the doctor’s office or clinic setting. That means it doesn’t involve surgery, sedation, or anesthesia, and no downtime is needed afterward. You stay awake and alert throughout the treatment.
During your TMS treatment, the clinician will seat you in a comfortable chair, provide you with earplugs, and then place a magnetic coil on your head near the area of the brain to be treated. In the case of depression, this area is called the left dorsolateral prefrontal cortex, just above the left eyebrow.
If being treated for other conditions, the treatment location may be different and is determined by the doctor or nurse practitioner in the initial treatment session, referred to as the ‘mapping’ session. During a typical treatment session:
Short electromagnetic pulses are administered through the coil. The magnetic pulses easily pass through your skull and cause small electrical currents that stimulate nerve cells.
- You’ll hear clicking sounds and feel a tapping or tingling sensation on your head during each treatment
- You may feel some scalp discomfort during the treatment and for a short time afterward, but this typically subsides after the first few treatments as the scalp desensitizes.
After TMS procedure
Upon completion of your treatment, you’re able to go straight back into your day, drive back to work or home, and continue on as normal. About 1 in 15 patients report painful scalp sensations or facial twitching during the magnetic pulses, which also tend to diminish over the course of the treatment. Repositioning the coil and adjusting the stimulation settings can also help to reduce these mild side effects.
There are no known complications
The most serious risk of TMS is the possibility of producing a seizure—but the risk is very small at around .001%. There have only been a few documented cases of seizures occurring due to TMS treatment, which is generally due to a person having a low seizure threshold. If you have a high risk of seizure, such as epilepsy, head injury, anorexia, or alcohol use disorder, you’re unlikely to be a candidate for TMS.
Unlike the oldest brain stimulation therapy, electroconvulsive therapy (ECT), TMS has no effect on memory or mental clarity and does not cause muscle aches, spasms, or other undesired side effects. It also avoids the negative side effects of sedation required for ECT. The only side effects associated with TMS include temporary scalp discomfort and headaches. While about 1 in 15 TMS patients report a slight headache, typically relieved with over-the-counter medications and tends to diminish over the course of treatment.